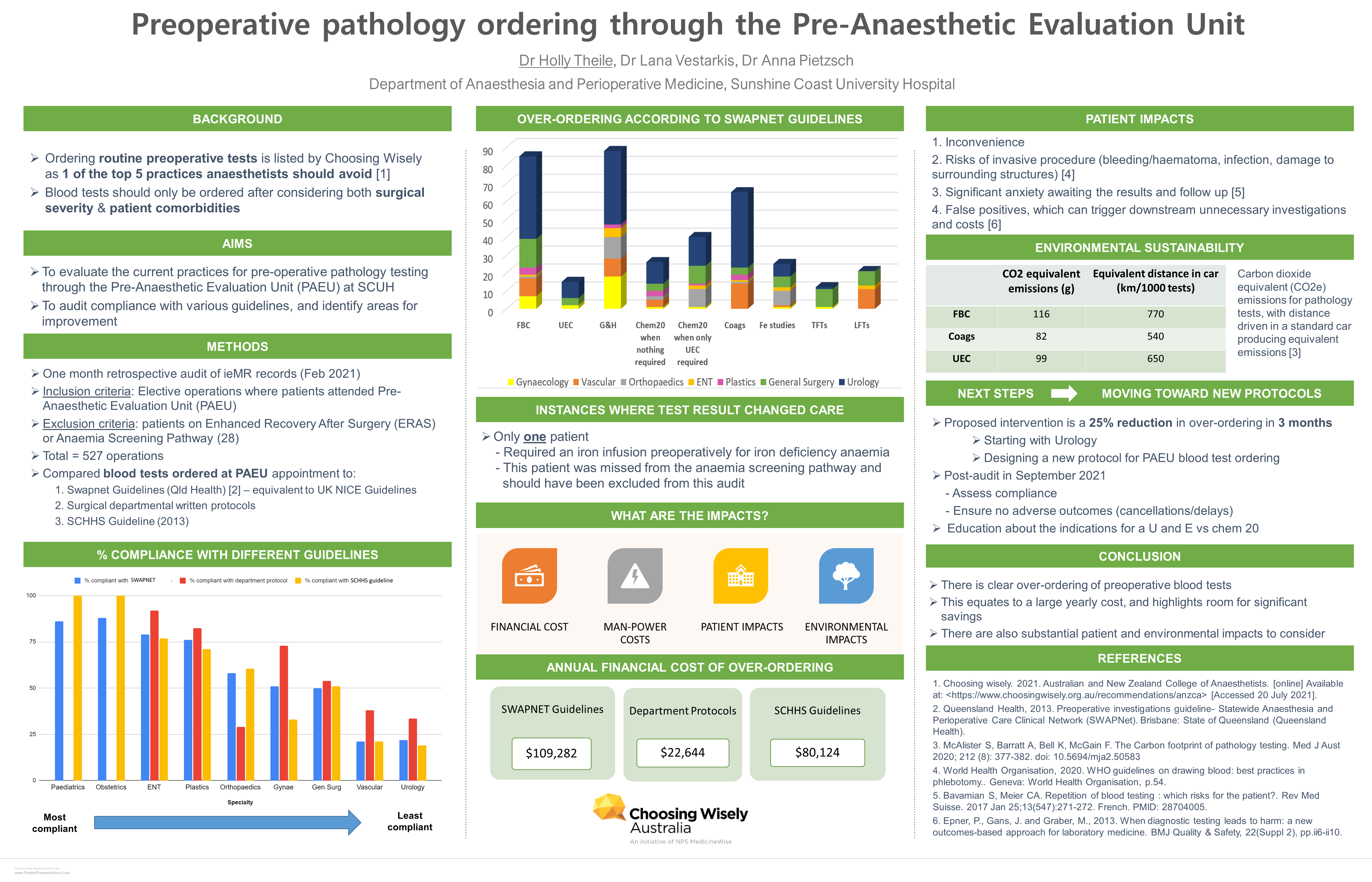
We undertook an audit of preoperative blood tests performed at the Sunshine Coast University Hospital over a one-month period in February 2021, and compared this to local protocols and Queensland-wide evidence-based guidelines.
The results demonstrated that our local practice deviated significantly from evidence-based guidelines, and also interestingly from our own local protocols. Of the 527 patients, 41% had incorrect pathology ordered. On breaking this down by speciality, there were four departments in which over ordering of pathology occurred for more than 50% of patients. For our urology patients, 77% received blood tests that were not supported by evidence-based guidelines.
Over this one month period, the only changes to care that resulted from the overordering of blood tests were two sets of blood tests that were repeated on the day of surgery, and an iron infusion for a patient who had been missed by the anaemia screening pathway and should have been excluded from the audit. This showed us that we had the potential to reduce unnecessary pathology tests without harming patients.
The impact of these unnecessary blood tests extends beyond the dollar value which we estimated to be $109,000 over a 12-month period. There was also time lost by patients, the distress and pain of blood tests and valuable staff time spent on ordering, performing, and following up pathology results. By reducing unnecessary testing, we can free up resources that may be utilised for other important services. Additionally, as a department with a strong sustainability focus, the CO2 emissions generated from unnecessary blood tests was substantial.